 At this point she was able to tolerate a rectal exam, during which, I found hypertension in the anal sphincter and and levator ani muscles (a group of muscles which starts at the pubic bone and circle around the vagina and rectum). Afterwards, she noted decreased pain when in the car and was able to sit more upright. She received a steroid injection between her second and third visits. Michelle was very dedicated to her home exercise program and reported getting the most relief from foam rolling her glutes. 
She also performed diaphragmatic breathing exercises to help restore the natural movement of her pelvic floor muscles. For more details, check out What’s The ‘Right’ Way To Poop? I advised Michelle to start foam rolling her legs and hips and to perform several stretches at home to help relax the pelvic floor muscles and several of the other muscles that attach to the pelvis. I provided education on proper mechanics when having a bowel movement to prevent straining which would make her pelvic floor muscles even tighter. Once this was achieved, we could start working on strengthening and motor control exercises for the pelvic floor to address Michelle’s urinary leakage. Our initial goal was to focus on decreasing restrictions in her muscles and connective tissue to allow the pelvic floor muscles to better relax and lengthen. Together we decided to start with a weekly PT session. For a double whammy, these tight muscles were not able to effectively contract when she sneezed, ran, or jumped, which caused urinary leakage, known as stress incontinence. Some other things that likely contributed to her pain were the physical stress of two pregnancies and vaginal deliveries, intermittent straining to have a bowel movement, as well as altered posture and biomechanics resulting from the pain. Plan: I suspected that due to Michelle’s hypermobile tailbone, her muscles became very tense to stabilize this joint. I discovered that her pelvic floor muscles were tight and weak and she had difficulty relaxing them. I assessed Michelle’s pelvic floor muscles vaginally instead of rectally because of her previous painful experience in PT. I also found restrictions in the connective tissue of her abdomen, low back, posterior hips, posterior thighs, and perineum. I found muscular restrictions throughout her gluteal muscles, hamstrings and deep hip flexors. Due to the severity of her pain, Michelle and I decided it would be beneficial to receive one more injection to help her tolerate therapy, but I warned that it was important to continue with therapy even after the pain decreased to ensure long lasting results.Įxamination: When I examined Michelle, I noticed that she shifted her weight from side to side and leaned back to avoid putting direct pressure on her tailbone. I believed that the injections were helping with the pain in the short term, but did not address restrictions in the muscles and connective tissues so once the injection wore off, the pain would return. She had significant relief with past corticosteroid injections, however had never paired it with PT. My first thoughts: Michelle had only briefly tried pelvic floor PT but had stopped because it was too painful. When her symptoms returned about a year later, she received another injection, however she only had pain relief for six months. She stopped attending PT because she experienced relief with a corticosteroid injection. Michelle had participated in several pelvic floor physical therapy (PT) sessions around the initial onset of her symptoms, however they mainly consisted of mobilizing the tailbone and were very painful. She enjoyed doing high intensity aerobic exercise and yoga classes but had stopped due to incontinence and pain.Īn MRI several years ago showed a dislocated tailbone. Lastly, Michelle had experienced urinary leakage with running, jumping, and sneezing since delivering her two children. Using a cushion with a coccyx cut out and leaning forward helped improve sitting tolerance. Her symptoms were aggravated by sitting (especially in the car or on hard surfaces) or arching her back and alleviated by standing. Michelle reported sharp pain around the tailbone, which sometimes radiated to the side of her hips. 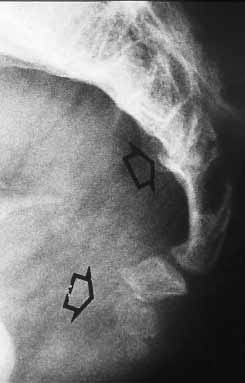 
For more on Coccydynia, see this blog post. Michelle did not know what caused the injury, but was working out a lot at the time of onset and thinks this may have contributed. Her symptoms started one year after giving birth to her second child, and had continued off and on for about three years. Michelle is a 39 year old patient who was referred to PHRC by her pain management specialist for evaluation and treatment of tailbone pain, known as Coccydynia. By Jennifer Keesee, PT, DPT, PHRC Westlake Village 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
